Hospital News
-

Stop the overdose before the first pill is ever taken
June 01, 2026Memorial Medical Center’s Medication Take Back Box located in our Emergency Room lobby provides a secure, anonymous, and dependable mechanism for safe disposal in our community.
Learn more -
Memorial Minute: May 29, 2026
May 29, 2026News from the leadership team at Memorial Medical Center.
Learn more -

Memorial Medical Center Names Andrew Cummins As 2026 Mercy Award Winner
May 22, 2026Las Cruces, New Mexico — May 22, 2026 — Memorial Medical Center is proud to announce that Andrew Cummins, Director of Marketing & Communications, has been recognized as the hospital’s 2026 Mercy Award winner. The Mercy Award recognizes one employee from each of Lifepoint Health’s facilities who profoundly touches the lives of others and best…
Learn more -

Employee Spotlight: Pharmacy Tech Celebrates 20 Years At MMC & Nursing Degree – All At Once
May 20, 2026Nicole Chacon this month marked her 20th anniversary as a Pharmacy Technician at Memorial Medical Center’s annual Employee Service Awards, earned her nursing degree from New Mexico State University, and accepted a new job as a registered nurse in Memorial’s bustling Emergency Department.
Learn more -

A Month to Celebrate the People Who Make Care Possible
May 11, 2026For more than 75 years, Memorial Medical Center has served this community through times of growth, challenge, and change. That enduring legacy is built not on buildings or equipment alone, but on generations of physicians, nurses, staff, and community partners who have shared a commitment to caring for our neighbors when they need it most.
Learn more -

Southern New Mexico Family Medicine Residency Program Welcomes Resident Class of 2029
May 05, 2026This talented group of eight physicians will begin their graduate medical education journey in Las Cruces in June 2026.
Learn more -
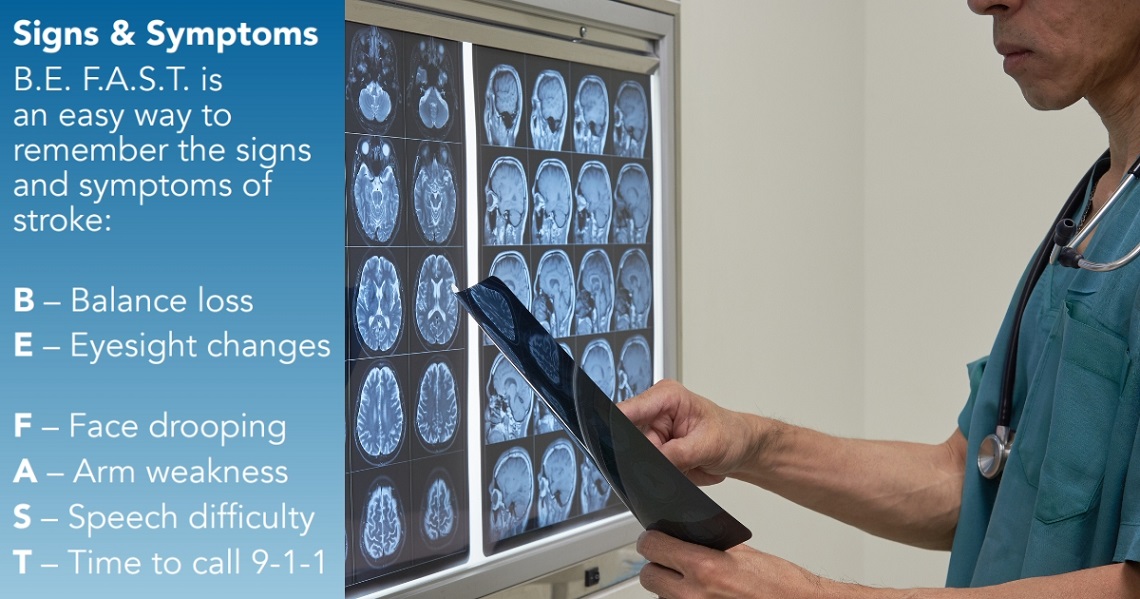
Stroke Awareness Month: Time Lost Is Brain Lost
May 04, 2026Fast action can make all the difference.
Learn more -

Setting The Standard In Healing: Memorial Wound Care Center Again Earns National Awards
April 14, 2026These honors reflect the team’s unwavering commitment to exceptional patient care, clinical expertise, and delivering the highest standard of healing every day for community members across Southern New Mexico.
Learn more -
Memorial Minute: April 14, 2026
April 14, 2026News from the leadership team at Memorial Medical Center.
Learn more -

Breathe Better This Spring: How Allergies Affect Your Sleep
April 08, 2026When spring arrives, many of us start sneezing and sniffling. But did you know that spring allergies can also change how you breathe while you sleep?
Learn more -

Employee Spotlight: Samantha Chavez, RN, Neonatal Intensive Care Unit
March 17, 2026She's En Pointe: Nurturing Lives In The NICU & On The Dance Floor
Learn more -

Specializing In You: Helping A Community Icon
March 09, 2026Las Cruces icon Wanda Bowman is pursing even more hopes, dreams and travels after a total knee replacement with Dr. Robert Schwartz at MMC.
Learn more -

New System Provides Patients with Fast and Secure Access to Medical Imaging Records
March 03, 2026With this new free service, patients can now access, store, and share all of their Memorial Medical Center imaging records anytime, on any device, in just a few clicks.
Learn more -
Memorial Minute: February 27, 2026
February 27, 2026News from the leadership team at Memorial Medical Center.
Learn more -

Saeed Shojaee Named MMC Laboratorian of the Year
February 11, 2026Please join us in congratulating Saeed Shojaee on being selected as this year’s Memorial Medical Center Laboratorian of the Year. The recognition comes as no surprise to those who work alongside him every day. Known for his dedication, positive attitude, and willingness to step in wherever needed, Saeed embodies what it means to be a true team player.
Learn more -

Calcium scoring: What a 15-minute test can tell you about your heart health
February 02, 2026As many of us know, numbers can tell us plenty about our heart health and where it’s headed – from blood pressure to cholesterol to blood sugar. For some people, one key painless and non-invasive test is a cardiac calcium scoring CT.
Learn more -

Healthy Habits to Start in 2026 for Better Overall Health
January 19, 2026The beginning of a new year offers a natural opportunity to reassess your health and build habits that help you feel better and stay healthier over time. While big resolutions can feel overwhelming or short-lived, the most effective changes usually come from small, sustainable strategies that are easier to maintain. In Las…
Learn more -

MMC Milestone: Dr. Fontan Celebrates 1,000th Robotic-Assisted Surgery
January 16, 2026Congratulations to Fermin Fontan, MD, FACS, FASMBS, on reaching the milestone of 1,000 robotic-assisted surgical cases at Memorial Medical Center.
Learn more -
Memorial Minute: January 15, 2026
January 15, 2026News from the leadership team at Memorial Medical Center.
Learn more -

What Your Annual Blood Work Can Reveal About Your Health
December 22, 2025Your yearly blood work gives your provider information they can’t see during a physical exam, sometimes before you notice any symptoms at all. Blood work isn’t only for sick visits – routine lab work plays a key role in preventive care and long-term health. In Las Cruces, New Mexico, many…
Learn more
